- Unveiling Novel Genetic Mutations and Prognostic Indicators in Breast Carcinoma: An Analysis of The Cancer Genome Atlas (TCGA) Data Cureus
- Whole-genome landscapes of 1,364 breast cancers Nature
- Inocras, Samsung Medical Center and Seoul St. Mary’s Hospital Researchers Publish Groundbreaking Study with 1,364 Whole-Genomes of Breast Cancer in Nature Business Wire
Category: 3. Business
-
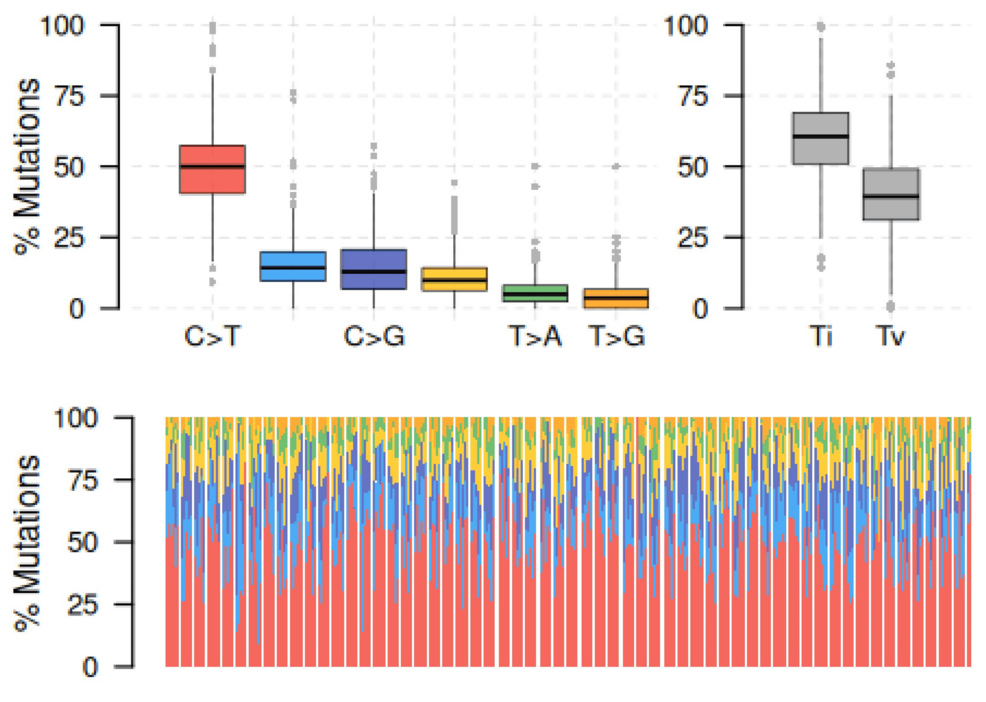
Unveiling Novel Genetic Mutations and Prognostic Indicators in Breast Carcinoma: An Analysis of The Cancer Genome Atlas (TCGA) Data – Cureus
-

Does Silver Tiger Metals’ C$40 Million Raise Reframe Its Funding Risk or Dilution Trade-Offs (TSXV:SLVR)?
-
Silver Tiger Metals Inc. recently completed a follow-on equity offering of C$40.00 million, issuing 54,800,000 common shares at C$0.73 each under Regulation S and Rule 144A, alongside reporting a smaller quarterly net loss of C$0.92 million.
-
This capital raise, combined with slightly lower losses per share and increased visibility through mining investment conferences, meaningfully reshapes how investors may view the company’s funding position and project ambitions.
-
We’ll now explore how the sizeable C$40.00 million equity raise influences Silver Tiger Metals’ investment narrative and future project optionality.
Uncover the next big thing with financially sound penny stocks that balance risk and reward.
To own Silver Tiger Metals, you need to believe that the El Tigre Stockwork silver-gold project can transition from permits and studies into a viable mine, while the company manages dilution and execution risk. The recent C$40.00 million equity raise, on top of earlier offerings, materially reinforces the funding side of that story and may ease near term concerns about how to advance construction after securing Mexican environmental approvals. At the same time, it amplifies the central trade off for shareholders: the company has more capital to push El Tigre forward, but existing investors now share that upside across a much larger share base. Near term catalysts still hinge on project financing milestones, construction decisions and any updates on economics, while key risks remain cost inflation, permitting or build delays and continued reliance on equity markets if spending runs ahead of plan.
However, this extra capital also sharpens a dilution risk that investors should not ignore. Despite retreating, Silver Tiger Metals’ shares might still be trading above their fair value and there could be some more downside. Discover how much.
TSXV:SLVR Community Fair Values as at Dec 2025 Seven Simply Wall St Community fair value views span roughly C$3.30 to a very large C$33.00, underlining how far opinions diverge on Silver Tiger’s upside. Set that against the recent heavy equity issuance and project execution risk, and it becomes clear why you may want to weigh several viewpoints before forming your own stance on the shares.
Explore 7 other fair value estimates on Silver Tiger Metals – why the stock might be a potential multi-bagger!
Disagree with this assessment? Create your own narrative in under 3 minutes – extraordinary investment returns rarely come from following the herd.
Continue Reading
-
-
Fixed-Duration Epcoritamab Plus Chemotherapy Yields Response, Remissions in DLBCL
At the
American Society of Hematology (ASH) 2025 meeting, updated results from the phase 2 EPCORE NHL‑2 (NCT04663347) trial highlighted the potential of epcoritamab combined with chemotherapy to improve outcomes for patients with newly diagnosed diffuse large B-cell lymphoma (DLBCL), spanning both high-risk and frail or older populations.The EPCORE NHL‑2 trial phase 1b/2 enrolled adults with newly diagnosed CD20-positive DLBCL who were ineligible for full-dose R‑CHOP due to age (75 years and older) or age 65 years and older with significant comorbidities.1 Patients received a fixed-duration regimen of subcutaneous epcoritamab 48 mg combined with R‑mini‑CHOP. Epcoritamab was administered weekly in cycles 1–2, every 3 weeks in cycles 3–6, and every 4 weeks in cycles 7–8, with step-up dosing during the cycle. The primary end point was overall response rate (ORR). Secondary end points included minimal residual disease (MRD) negativity, assessed using the AVENIO Oncology circulating tumor DNA (ctDNA) assay, with MRD negativity defined as less than 1 mutant molecule/mL. Safety, treatment completion, and relative dose intensity of R‑mini‑CHOP were also evaluated.
As of April 9, 2025, 28 patients received epcoritamab plus R-mini-CHOP. Median (IQR) age was 81 (74, 90) years. Most patients (79%) completed treatment, with a median R-mini-CHOP dose intensity of 94% or greater. ORR was 89% and the CR rate was 86%, while the median duration of response and complete response (CR) were not reached. Estimated 2-year progression-free survival (PFS) and overall survival (OS) were 76% and 82%, respectively. MRD negativity was achieved in 95% of evaluable patients, including 93% with International Prognostic Index (IPI) 3 through 5 and 89% with bulky disease; 86% of patients MRD-negative at C3D1 sustained negativity through C6D1. Grade 3 or greater infections occurred in 29% of patients, and 11% discontinued epcoritamab due to treatment-emergent adverse events.
In the second analysis, patients received fixed-duration epcoritamab in combination with 6 cycles of standard R‑CHOP, followed by epcoritamab monotherapy for up to 1 year.2 Epcoritamab was administered subcutaneously with step-up dosing during cycle 1 and weekly in cycles 1–4, then every 3 weeks in cycles 5–6, with subsequent monthly monotherapy. The study evaluated efficacy using investigator-assessed ORR as the primary end point. Secondary end points included CR rate, duration of response, PFS and OS, safety, and tolerability. MRD negativity was also assessed.
A total of 47 patients received epcoritamab plus R‑CHOP. Median age was 64 (19, 82) years. IPI scores were 3 in 57% of patients and 4–5 in 38%. After a median follow-up of 38.8 (0.8, 44.3) months, ORR was 98% and CR rate was 85%, with 67% of responses and 75% of CRs ongoing at 33 months.
High CR rates were observed across subgroups (IPI 3, 86% vs IPI 4-5, 83%), age, tumor size, and cell of origin. By cycle 3 day 1, 86% of MRD-evaluable patients were MRD negative, with sustained reductions in ctDNA through cycle 6 day 1. Most patients (94%) completed 6 cycles of R‑CHOP, and 68% completed treatment as planned; among these, 30 of 32 patients had a CR, with 87% maintaining response at a median 25.3-month follow-up. Safety was consistent with prior reports, with serious or grade 3 or greater infections primarily in the first 6 months and no new grade 5 events reported.
References
1. Cheah C, Belada D, Darrah J, et al. Epcoritamab plus R-mini-CHOP results in 2-year remissions and high MRD negativity rates in elderly patients with newly diagnosed DLBCL: Results from the EPCORE NHL-2 trial. Presented at: ASH 2025; December 6-9, 2025; Orlando, Florida. Poster 64
2. Falchi L, de Vos S, Brody J, et al. Fixed-duration epcoritamab plus R-CHOP in patients with newly diagnosed DLBCL and high IPI scores (3–5) led to sustained remissions and disease-free survival beyond 3 years: Results from the EPCORE NHL-2 trial. Presented at: ASH 2025; December 6-9, 2025; Orlando, Florida. Poster 1955
Continue Reading
-
Epcoritamab Combo Significantly Improves Efficacy in 2L R/R Follicular Lymphoma
Fixed-duration epcoritamab (Epkinly) plus rituximab (Rituxan) and lenalidomide (Revlimid; R2) demonstrated significant improvements in progression-free survival (PFS) and response rates compared with R2 alone in patients with relapsed/refractory follicular lymphoma, according to findings from the phase 3 EPCORE FL-1 trial (NCT05409066) presented in a press briefing during the
2025 American Society of Hematology (ASH) Annual Meeting and Exposition .1,2At a median follow-up of 14.8 months, results showed that the median PFS per independent review committee (IRC) was not estimable with epcoritamab (95% CI, NE-NE) plus R2 compared with 11.7 months (95% CI, 11.1-15.1) with R2 alone, leading to a 79% reduction in the risk of disease progression or death (HR, 0.21; 95% CI, 0.14-0.31; P <.0001). The concordance rate was 94% for PFS between IRC and investigator assessment. The estimated 16-month PFS rates were 85.5% (95% CI, 79.7%-89.7%) and 40.2% (95% CI, 31.8%-48.4%), respectively.
The epcoritamab regimen elicited a 95% objective response rate (ORR) compared with 79% with R2 alone (P <.0001). In the epcoritamab arm, the complete response (CR) rate was 83% and the partial response (PR) rate was 12%; 1 patient had stable disease (SD), 3% of patients had progressive disease (PD), and 2% were not evaluable. In the R2 arm, the CR rate was 50% and the PR rate was 29%; 7% of patients each had SD, PD, and were not evaluable.
“Epcoritamab and R2 is a novel chemotherapy-free, fixed-duration therapy that is suitable for outpatient administration, and we believe sets a new benchmark as standard of care for second-line [and beyond] follicular lymphoma,” lead study author Lorenzo Falchi, MD, of the Lymphoma Service at Memorial Sloan Kettering Cancer Center in New York, NY, said in the oral presentation. “We’re happy to see that the FDA granted full approval to epcoritamab and R2 on November 18, 2025, for [this patient population].”
R2 is the only second-line alternative to chemoimmunotherapy-based treatment for patients with relapsed/refractory follicular lymphoma. The FDA initially approved epcoritamab, a CD3xCD20 bispecific antibody, as a single agent for the treatment of patients with relapsed/refractory follicular lymphoma following at least 2 lines of systemic therapy.3
Early data from the phase 1b/2 EPCORE NHL-2 trial (NCT04663347), which evaluated fixed-duration epcoritamab plus R2 for relapsed/refractory follicular lymphoma, demonstrated deep and durable responses and a manageable safety profile.4
In November 2025, the
FDA also approved epcoritamab in combination with R2 in relapsed/refractory follicular lymphoma, based on the phase 3 EPCORE FL-1 findings, which is what Falchi presented during the press briefing.5 In the international, open-label, EPCORE FL-1 trial, patients underwent a 1:1 randomization to receive fixed-duration epcoritamab at 48 mg plus R2 (n = 243) or R2 alone (n = 245).Epcoritamab was administered in a 3-step-up, 2-dosing schedule at 0.16 mg on day 1, 0.8 mg on day 8, and 3 mg on day 15, all in cycle 1. Cycles 2 and 3 were administered weekly, and cycles 4 to 12 were administered every 4 weeks. Rituximab was given at 375 mg/m2 for 5 cycles; the agent was given weekly in cycle 1 and every 4 weeks in cycles 2 through 5. Lastly, lenalidomide was given at 20 mg for 12 cycles; treatment was given daily in cycles 1 through 12 on days 1 through 21.
The dual primary end points were ORR and PFS, both per IRC; key secondary end points were CR rate per IRC, overall survival (OS), and minimal residual disease. Additional secondary end points were duration of response (DOR), duration of complete response, time to next lymphoma treatment (TTNLT), safety, and patient-reported outcome assessments.
The data cutoff date was May 24, 2025, and patients were enrolled between October 2022 and January 2025.
To be eligible for enrollment, patients had to have histologically confirmed CD20-positive follicular lymphoma that was grade 1 to 3a and stage II to IV. At least 1 prior treatment was required, including an anti-CD20 monoclonal antibody plus an alkylating agent, and at least 1 Groupe d’Etude des Lymphomes Folliculaires criterion needed to be met.
Patients were stratified by disease status in second line (> or ≤ 2 years since last therapy), third line (> or <6 months since last therapy), and region (US/EU vs rest of world).
Baseline characteristics showed that the median age was 61 years (range, 24-89), and 40% of patients were at least 65 years old; 57% of patients were male, and 72% were White. Thirty-one percent of patients had an ECOG performance status of 1 to 2, while 83% had Ann Arbor stage III to IV disease. Regarding Follicular Lymphoma International Prognostic Index, the breakdown of scores was 0 to 1 (24%), 2 (32%), and 3 to 5 (44%). Twenty-two percent of patients had bulky disease, consisting of at least 7 cm.
The median time from initial diagnosis to randomization was 5 years (range, 0.1-43.0), and the median number of prior lines of therapy was 1 (range, 1-7), with most patients receiving 1 (59%), 2 (24%), or at least 3 (17%). All patients received a prior anti-CD20 antibody, and 3% had received prior R2. Forty-one percent of patients experienced disease progression within 2 years from starting frontline therapy; 34% of patients were refractory to their first-line therapy, and 37% of patients had double-refractory disease.
Additional efficacy data showed that the median DOR with epcoritamab plus R2 was NE (95% CI, NE-NE) compared with 11.5 months (95% CI, 8.5-18.6) with R2 alone (HR, 0.19; 95% CI, 0.12-0.30; P <.0001).
The epcoritamab regimen also extended TTNLT; the median was NE (NE-NE) compared with 24.3 months (95% CI, 18.2-NE) with R2 alone (HR, 0.15; 95% CI, 0.09-0.27; P <.0001). At 16 months, 92.8% of patients on epcoritamab plus R2 remained free from new anti-lymphoma therapy vs 64.9% of those on R2 alone.
Falchi noted there is a positive trend for OS with the epcoritamab arm, which is NE (95% CI, NE-NE) in both arms (HR, 0.38; 95% CI, 0.18-0.80; P = .0039), adding that there are 10 and 25 events in the epcoritamab and R2-alone arms, respectively. Sixteen-month estimates for OS were 95.8% for epcoritamab plus R2 vs 88.8% with R2 alone.
Regarding safety, any-grade adverse events occurred in 100% and 99% of patients on epcoritamab plus R2 and R2 alone, with grade 3 or higher AEs at 90% and 68%, respectively. Serious AEs occurred in 56% and 29%, respectively, and AEs that led to treatment discontinuation occurred in 19% and 12% of patients.
Any-grade and grade 3 or higher AEs of clinical interest occurring in at least 20% of patients on epcoritamab/R2 and R2 alone included infections (77% and 33% vs 53% and 16%), neutropenia (74% and 69% vs 52% and 42%), cytokine release syndrome (any-grade, 35% vs <1%) thrombocytopenia (28% and 9% vs 18% and 6%), pyrexia (24% and <1%; 14% and 1%), rash (24% and 8% vs 22% and 4%), and COVID-19 (22% and 3% vs 13% and 2%).
On the epcoritamab arm, 3% of patients discontinued due to neutropenia vs 2% in the R2-alone arm. Febrile neutropenia occurred in 6% and 3% of patients, respectively. Discontinuation rates due to infections occurred in 6% and 1% of patients, respectively.
Two percent and 4% of patients on epcoritamab and R2 and R2 alone experienced fatal AEs.
“Despite these higher rates of AEs in the epcoritamab and R2 arm, the median relative dose intensity was greater than 90%,” Falchi added.
Disclosures: Falchi cited consultancy, including expert testimony, with Johnson & Johnson, Roche, ADC Therapeutics, Evommune, F. Hoffman-La Roche Ltd., AbbVie, Sanofi, Genentech, AstraZeneca, Seagen, Merck, and Genmab; honoraria from Roche, Kite Pharma, F. Hoffman-La Roche Ltd., AbbVie, and Genmab; and research funding from Roche, F. Hoffman-La Roche Ltd., AbbVie, Innate Pharma, Genentech, BeiGene, AstraZeneca, and Genmab.
References
- Falchi L, Nijland M, Huang H, et al. Primary phase 3 results from the EPCORE- FL-1 trial of epcoritamab with rituximab and lenalidomide (R2) versus R2 for relapsed or refractory follicular lymphoma. Blood. 2025;146(supplement 1):466. doi:10.1182/blood-2025-466
- Falchi L, Nijiland M, Huang H, et al. Epcoritamab, lenalidomide, and rituximab versus lenalidomide and rituximab for relapsed/refractory follicular lymphoma (EPCORE FL-1): a global, open-label, randomised, phase 3 trial. Lancet. Published online December 7, 2025. doi:10.1016/50140-6736(25)02360-8
- EPKINLY™ (epcoritamab-bysp) injection prescribing information. FDA. Updated May 2023. Accessed December 7, 2025. https://tinyurl.com/mrvfmaur
- Falchi L, Sureda A, Leppä S, et al. Fixed-duration epcoritamab plus R2 drives favorable outcomes in relapsed or refractory follicular lymphoma. Blood. 2025;146(22):2629-2640. doi:10.1182/blood.2025029909
- FDA approves epcoritamab-bysp for follicular lymphoma indications. News release. FDA. November 18, 2025. Accessed December 7, 2025. https://tinyurl.com/y8t4hh3a
Continue Reading
-

Grotmas Calendar Day 7 – Embrace the tragic madness of the Blood Angels with a new Detachment
The Red Thirst and the Black Rage will forever be the twin spiritual curses that the Blood Angels must hide from their allies for fear of censure. However, they can prove potent weapons of last resort when unleashed upon a determined foe. No Blood Angel takes such a decision lightly: to the sons of Sanguinius, a victory won through giving in to their Red Thirst is tainted at best, whilst to succumb to the Black Rage is no better than a living death. All this is little comfort to enemies facing the Blood Angels’ onslaught in such moments, however. Power-armoured killers pound across the battlefield, shrugging off incoming fire as they close the distance with terrifying haste. Blood detonates from each crunching charge as the sons of Sanguinius rip their victims apart or carve them into gory ruin. At the very heart of the battle, the lost brethren of the Death Company fight with even greater fury, a whirlwind of rage-fuelled savagery that can end only with their deaths or those of all their foes.
Continue Reading
-

Brookfield, GIC near binding offer for National Storage, Bloomberg News reports
Dec 7 (Reuters) – Brookfield Asset Management (BAM.N) and Singapore’s GIC are nearing a binding offer for National Storage REIT (NSR.AX) in a deal that may value the Sydney-listed company at about 4 billion Australian dollars ($2.65 billion), Bloomberg News reported on Sunday, citing people familiar with the matter.The parties are finalizing details of the deal that could be announced as soon as Monday, the report said, adding that, Brookfield and GIC have successfully made progress on due diligence on National Storage.
Sign up here.
According to the report, the price of the binding offer is likely to be the same as a conditional one in November.
Reuters could not immediately verify the report.
Last month, National Storage REIT (NSR.AX) said it had received a A$4.02 billion buyout offer from a consortium of Brookfield and Singapore’s GIC in what would be the country’s biggest real estate privatisation deal.($1 = 1.5067 Australian dollars)
Reporting by Abu Sultan in Bengaluru; Editing by Andrea Ricci
Our Standards: The Thomson Reuters Trust Principles.
Continue Reading
-

Pakistan’s crypto deal with Binance & why Asim Munir, even ISI are ‘in the picture’
New Delhi: Pakistan is going all out on crypto, and it’s not merely an economic step but also a deeply political one in which the country’s military and intelligence seem involved too.
A day after he was elevated as the country’s most powerful commander yet, Army Chief and Chief of Defence Forces Field Marshal Asim Munir joined Prime Minister Shehbaz Sharif and Inter-Services Intelligence (ISI) chief Asim Malik in a high-profile meeting in Islamabad with crypto firm Binance’s CEO Richard Teng.
Also seen with them was Bilal Bin Saqib, chairman of the newly formed Pakistan Virtual Assets Regulatory Authority (PVARA), who briefed them on Pakistan’s National Digital Assets Framework.
Pakistan’s Ministry of Finance later said that the meeting, which also had senior Binance executives in attendance, focused on building a “secure, transparent and innovation-driven digital asset ecosystem” in the country.
Binance Senior Leadership Visits Pakistan as Government Signals Strong Commitment to Digital Asset Regulation
Senior leadership from @binance, including Global CEO @_RichardTeng, visited Islamabad for high-level engagements with Pakistan’s top leadership.
The meeting was… pic.twitter.com/vAh2WoMhg7
— Pakistan Crypto Council (@cryptocouncilpk) December 6, 2025
The meeting and the finance ministry’s assertion came even as local banks have been raising the alarm against the crypto push in Pakistan.
According to a Dawn report, at a consultative meeting convened Friday by the finance ministry and PVARA, Pakistan’s top banks expressed concern about money laundering, compliance risks, and global precedents where crypto-related gaps triggered major regulatory penalties.
Yet, the government appears determined to move forward.
According to the report, the government has now floated a “time-bound amnesty” allowing crypto traders, who handle more than $250 billion in annual turnover, to shift assets onto regulated platforms with no penalty.
A Binance representative told participants that Pakistani users hold around $5 billion on Binance alone, and argued that tokenised assets should be counted as part of Pakistan’s “liquid money supply”, according to the Dawn report.
“Liquid money supply” includes assets that can be easily and immediately used as a medium of exchange for transactions.
The Dawn reported that they were told, according to those present at the meeting, that Binance could provide real-time reporting, enable banks to lend against digitally verified collateral, and help Pakistan attract billions of dollars in new inflows, including new remittance routes that could sit atop the $38-billion Pakistan receives annually from overseas workers.
Banks, however, asked whether expecting such visibility and traceability was realistic.
Also Read: Pakistan’s $21 billion crypto market is out of the shadows. It’s finally legal there
Pakistan’s crypto rush
Crypto is officially banned for financial institutions in Pakistan, but it is allowed as legal tender.
In February, the Pakistani government established a Crypto Council. In May, the government shifted towards legalisation with proposals to regulate it as an economic lifeline through a formal, legal framework.
Also, the Crypto Council was elevated to a full-fledged regulatory body named the Pakistan Digital Assets Authority, tasked with overseeing and regulating digital assets, including cryptocurrencies and blockchain technologies.
Before that, in April, Pakistan entered into a partnership with World Liberty Financial (WLF), a firm reportedly connected to members of Trump’s family. WLF has pledged support in helping Pakistan develop blockchain infrastructure, tokenise assets, and navigate the broader crypto industry. However, the specifics of the agreement remain unclear.
Then in July, the Virtual Assets Ordinance 2025 came into force for establishing a regulatory and sandbox environment through the creation of Pakistan Virtual Assets Regulatory Authority (PVARA), the national regulator for virtual assets in Pakistan which would be independent.
The State Bank of Pakistan (SBP), the country’s central bank which had banned crypto, announced in September that it would withdraw its earlier advisory against cryptocurrencies and begin formal legalisation.
It then announced it was drafting a central bank digital currency (CBDC) and coordinating with lawmakers on the Virtual Assets Act 2025, which will create a fully regulated framework for digital asset trading.
But why did the government move to regulate and legalise crypto so hurriedly—all within a year?
For Pakistan, crypto could offer a potential workaround to its known structural economic constraints—from slow banking systems to chronic foreign exchange shortages. Tokenised assets and remittance rails could ideally unlock new inflows.
From the point of view of Binance, Pakistan has 40 million Binance users, making it one of its biggest untapped regulated markets. A State-backed embrace of crypto could cement Binance’s dominance at a moment when its US legal troubles threaten its global footprint.
And, there could be a US angle, a Chinese and a military push to it too.
Binance–Trump–Pakistan triangle
Looming over Pakistan’s crypto pivot is the global controversy surrounding Binance and its Chinese founder Changpeng Zhao (CZ), who maintains a 90 percent stake in the company.
Zhao, who pleaded guilty in 2023 to failing to implement the US anti-money-laundering law at Binance and served several months in jail, received a presidential pardon from Donald Trump last month—a move Trump later claimed he barely recalled.
The pardon came shortly before Zhao deepened his engagement with Pakistan. In early 2025, Islamabad appointed him strategic adviser to the Pakistan Crypto Council, and several of Pakistan’s new crypto institutions, including the Pakistan Digital Assets Authority, were reportedly shaped with his input.
The relationship also intersects with the Trump family’s own crypto portfolio. Their company, World Liberty Financial (WLF), launched the USD1 stablecoin using code reportedly written with Binance’s help. Binance then promoted USD1 to its vast global user base, helping accumulate more than $2 billion worth of deposits that generate multimillion-dollar yields for Trump-linked interests.
Pakistan has since signed a “letter of intent” with WLF to cooperate on blockchain infrastructure and stablecoin integration. Bilal Bin Saqib, Pakistan’s key crypto architect, is also an adviser to WLF.
(Edited by Ajeet Tiwari)
Also Read: Crypto, crisis & the Trump connection: All about Pakistan’s new Virtual Assets Act
Continue Reading
-
Gintemetostat Shows Early Activity and Manageable Safety in Triple-Class Refractory Multiple Myeloma
Early data from the phase 1 trial (NCT05651932) of the MMSET/NSD2 inhibitor gintemetostat (KTX-1001) revealed that the agent was tolerable and produced encouraging antitumor activity in a heavily pretreated population of patients with relapsed or refractory multiple myeloma, including those with triple-class–refractory disease and high-risk features such as t(4;14). These results were presented at the
2025 ASH Annual Meeting , and Exposition.Among 40 patients treated with gintemetostat, 1 patient had a very good partial response, 1 patient had a partial response, 2 patients had a minimal response, and 12 patients had stable disease.
“Single-agent activity was demonstrated in heavily pretreated R/R multiple myeloma including t(4;14) positive patients across different dose-escalation cohorts,” said lead author Saad Usmani, MD, MBA, chief of Myeloma Service at Memorial Sloan Kettering Cancer Center.
Safety and Tolerability
The safety profile from the phase 1 study showed that 75% of patients experienced treatment-emergent adverse events (TEAEs) potentially related to gintemetostat and 45% experienced grade 3 or higher potentially gintemetostat-related TEAEs. Three patients had TEAEs that required a dose reduction.
Twelve patients remained on treatment at the data cutoff date of June 13, 2025. Of the 28 patients who discontinued treatment, progressive disease was the cause for 82%, physician decision for 7.1%, consent withdrawal for 7.1%, and TEAE for 3.6% (1 patient).
The most common grade 3/4hematologic TEAEs were thrombocytopenia (grade 3, 10%; grade 4, 20%), anemia (25%; 0%), neutropenia (25%; 5%), and febrile neutropenia (5%; 0%). The most common grade 3 nonhematologic TEAEs were infections (12.5%) and fatigue (10%).
There were 2 patient deaths, both of which were not related to gintemetostat treatment. One patient death was due to respiratory failure and the other was due to pleural effusion.
Study Background, Design, and Patient Characteristics
Regarding the rationale for the study, Usmani explained, “Overexpression of MMSET—also known as NSD2—often results from t(4;14) and is associated with poor clinical outcomes in patients with multiple myeloma.”
Accordingly, Usmani et al sought to explore the safety and efficacy of gintemetostat, an oral, first-in-class, potent and selective inhibitor of MMSET4 in patients with R/R multiple myeloma.
The ongoing, open-label, multicenter phase 1 dose escalation/expansion study of gintemetostat has accrued 40 patients with R/R multiple myeloma. The study is enrolling patients aged ≥18 years with R/R multiple myeloma who have received at least 3 prior therapies, including a proteasome inhibitor (PI), an immunomodulatory drug (IMiD), and an anti-CD38 monoclonal antibody.
The median age of the 40 patients in the dose-escalation phase was 69 years (range, 50–83) and 52.5% of patients were female. The ECOG performance status was 0 (22.5%) and 1 (77.5%). The median time since initial diagnosis was 8 years (range, 2–20). About one-third (32.5%) of patients had extramedullary disease and 30% had high-risk multiple myeloma per IMWG criteria.
Regarding cytogenetic abnormalities, 47.5% of patients had t(4;14), comprising 20% with t(4;14) with 1q+ or del(1p32), and 27.5% with t(4;14) alone. Further, 1 patient had t(14;20), 5 had 1q21 amplification, and 4 had del(17p).
The median number of prior lines of therapy was 6.5 (range, 3–25), with 77.5% of patients having received at least 5 lines of therapy. Seventy percent of patients had prior stem cell transplant.
Prior drug classes of therapy received included IMiD/PI (100%), anti-CD38 (98%), BCMA CAR-T (42.5%), BCMA-targeted bispecific antibodies (BsAb) and antibody-drug conjugates (57.5%), GPRC5D-targeted BsAb (32.5%), and FcRH5-targeted BsAb (7.5%). All patients except 1 were triple-drug exposed and 80% were penta-drug exposed.
Overall, 9 dose levels have been assessed using a 3+3 dose-escalation design. Gintemetostat is being administered orally in a 28-day cycle. Usmani did not provide the specific details of the what the different dose levels were.
Regarding pharmacokinetics, Usmani said, “Gintemetostat plasma concentrations increased with dose across all 9 dose levels tested, and at steady-state, moderate variability in exposure of gintemetostat was observed.”
Summary and Next Steps
In a news release accompanying the presentation at the ASH meeting, a statement from Usmani summarized the findings and next steps with gintemetostat.
“In the dose-escalation phase, gintemetostat monotherapy showed a favorable safety and tolerability profile and demonstrated disease control and efficacy. Pharmacodynamic data confirm target engagement, and we look forward to advancing into the dose-expansion phase to evaluate combinations with proteasome inhibitors, IMiDs, and next-generation CELMoDs such as mezigdomide,” stated Usmani.2
References
1. Usmani S, Bories P, Gasparetto C, et al. Phase 1 study of ktx-1001, a first-in-class oral MMSET/NSD2 inhibitor, demonstrates clinical activity in relapsed/refractory multiple myeloma. Blood. 2025;146(suppl 1): 250. doi:10.1182/blood-2025-250
2. K36 Therapeutics announces presentation of First-in-Human Clinical Data for Gintemetostat (KTX-1001) Demonstrating Target Engagement and Clinical Activity in Multiple Myeloma at ASH 2025 and the Appointment of Dr. Shinta Cheng, M.D., Ph.D., as Chief Medical Officer. Published online December 5, 2025. Accessed December 7, 2025.
https://tinyurl.com/3wzem4nx Continue Reading
-
Gintemetostat Has Single-Agent Activity in Pretreated R/R Multiple Myeloma
Preliminary activity and favorable safety were observed among patients with heavily pretreated, triple-class refractory, relapsed/refractory multiple myeloma who received single-agent gintemetostat (KTX-1001), according to a presentation on findings from a phase 1 study (NCT05651932) at the
2025 American Society of Hematology (ASH) Annual Meeting and Exposition. 1Among 40 patients treated with gintemetostat, 1 patient had a very good partial response, 1 patient had a partial response, 2 patients had a minimal response, and 12 patients had stable disease.
“Single-agent activity was demonstrated in heavily pretreated R/R multiple myeloma including t(4;14) positive patients across different dose-escalation cohorts,” said lead author Saad Usmani, MD, MBA, chief of Myeloma Service at Memorial Sloan Kettering Cancer Center.
Safety and Tolerability
The safety profile from the phase 1 study showed that 75% of patients experienced treatment-emergent adverse events (TEAEs) potentially related to gintemetostat and 45% experienced grade ≥3 potentially gintemetostat-related TEAEs. Three patients had TEAEs that required a dose reduction.
Twelve patients remained on treatment at the data cutoff date of June 13, 2025. Of the 28 patients who discontinued treatment, progressive disease was the cause for 82%, physician decision for 7.1%, consent withdrawal for 7.1%, and TEAE for 3.6% (1 patient)
The most common grade 3/4hematologic TEAEs were thrombocytopenia (grade 3, 10%; grade 4, 20%), anemia (25%; 0%), neutropenia (25%; 5%), and febrile neutropenia (5%; 0%). The most common grade 3 nonhematologic TEAEs were infections (12.5%) and fatigue (10%).
There were 2 patient deaths, both of which were not related to gintemetostat treatment. One patient death was due to respiratory failure and the other was due to pleural effusion.
Study Background, Design, and Patient Characteristics
Regarding the rationale for the study, Usmani explained, “Overexpression of MMSET—also known as NSD2—often results from t(4;14) and is associated with poor clinical outcomes in patients with multiple myeloma.”
Accordingly, Usmani et al sought to explore the safety and efficacy of gintemetostat, an oral, first-in-class, potent and selective inhibitor of MMSET4 in patients with R/R multiple myeloma.
The ongoing, open-label, multicenter phase 1 dose escalation/expansion study of gintemetostat has accrued 40 patients with R/R multiple myeloma. The study is enrolling patients aged ≥18 years with R/R multiple myeloma who have received at least 3 prior therapies, including a proteasome inhibitor (PI), an immunomodulatory drug (IMiD), and an anti-CD38 monoclonal antibody.
The median age of the 40 patients in the dose-escalation phase was 69 years (range, 50-83) and 52.5% of patients were female. The ECOG performance status was 0 (22.5%) and 1 (77.5%). The median time since initial diagnosis was 8 years (range, 2-20). About one-third (32.5%) of patients had extramedullary disease and 30% had high-risk multiple myeloma per IMWG criteria.
Regarding cytogenetic abnormalities, 47.5% of patients had t(4;14), comprising 20% with t(4;14) with 1q+ or del(1p32), and 27.5% with t(4;14) alone. Further, 1 patient had t(14;20), 5 had 1q21 amplification, and 4 had del(17p).
The median number of prior lines of therapy was 6.5 (range, 3-25), with 77.5% of patients having received at least 5 lines of therapy. Seventy percent of patients had prior stem cell transplant.
Prior drug classes of therapy received included IMiD/PI (100%), anti-CD38 (98%), BCMA CAR-T (42.5%), BCMA-targeted bispecific antibodies (BsAb) and antibody-drug conjugates (57.5%), GPRC5D-targeted BsAb (32.5%), and FcRH5-targeted BsAb (7.5%). All patients except 1 were triple-drug exposed and 80% were penta-drug exposed.
Overall, 9 dose levels have been assessed using a 3+3 dose-escalation design. Gintemetostat is being administered orally in a 28-day cycle. Usmani did not provide the specific details of the what the different dose levels were.
Regarding pharmacokinetics, Usmani said, “Gintemetostat plasma concentrations increased with dose across all 9 dose levels tested, and at steady-state, moderate variability in exposure of gintemetostat was observed.”
Summary and Next Steps
In a news release accompanying the presentation at the ASH meeting, a statement from Usmani summarized the findings and next steps with gintemetostat.
“In the dose-escalation phase, gintemetostat monotherapy showed a favorable safety and tolerability profile and demonstrated disease control and efficacy. Pharmacodynamic data confirm target engagement, and we look forward to advancing into the dose-expansion phase to evaluate combinations with proteasome inhibitors, IMiDs, and next-generation CELMoDs such as mezigdomide,” stated Usmani.2
References
- Usmani S, Bories P, Gasparetto C, et al. Phase 1 study of ktx-1001, a first-in-class oral MMSET/NSD2 inhibitor, demonstrates clinical activity in relapsed/refractory multiple myeloma. Blood. 2025;146(suppl 1): 250. doi:10.1182/blood-2025-250
- K36 Therapeutics announces presentation of First-in-Human Clinical Data for Gintemetostat (KTX-1001) Demonstrating Target Engagement and Clinical Activity in Multiple Myeloma at ASH 2025 and the Appointment of Dr. Shinta Cheng, M.D., Ph.D., as Chief Medical Officer. Published online December 5, 2025. Accessed December 7, 2025. https://tinyurl.com/3wzem4nx
Continue Reading
-

Ray Dalio warns that America is on track for a ‘debt death spiral.’ Are your assets safe?
Amal Alhasan / Getty Images Moneywise and Yahoo Finance LLC may earn commission or revenue through links in the content below.
The early 1970s were a turbulent time in America — marked by soaring inflation, an oil crisis and a sharp drop in stock prices that left investors scrambling for safe havens.
And, according to billionaire investor Ray Dalio, history may be repeating itself. Surging prices and massive government spending could prompt investors to once again question the value of fiat currencies and the paper assets tied to them (1).
“It’s very much like the early ’70s … where do you put your money in?” Dalio said at the Greenwich Economic Forum (2). “When you are holding money, and you put it in a debt instrument, and when there’s such a supply of debt and debt instruments, it’s not an effective storehold of wealth.”
Dalio has long warned about the sheer size of America’s national debt, now hovering around $37.86 trillion and climbing. He has described the situation as a potential “debt death spiral” — where the government must borrow just to pay the interest on existing debt. Over time, this process accelerates.
If that number feels abstract, Dalio has a more personal warning.
The asset he’s talking about is something nearly everyone holds in one way or another, whether in bank accounts or under mattresses: the U.S. dollar.
In a recent post on X, Dalio shared a Q&A with the Financial Times (3). When asked what would happen to bonds and the dollar if a politically weakened Federal Reserve lets inflation run hot, his answer was blunt:
“It would lead bonds and the dollar to go down in value and if not rectified, would lead to them being an ineffective storehold of wealth and the breaking down of the monetary order as we know it.”
That comment couldn’t have come at a more sensitive time for the Federal Reserve. President Donald Trump has repeatedly attacked Chair Jerome Powell and is searching for a replacement.
Treasury Secretary Scott Bessent told CNBC in late November, “I think there’s a very good chance that the president will make an announcement before Christmas … I think it’s time for the Fed just to move back into the background, like, it used to do, calm things down and work for the American people (4).”
Continue Reading