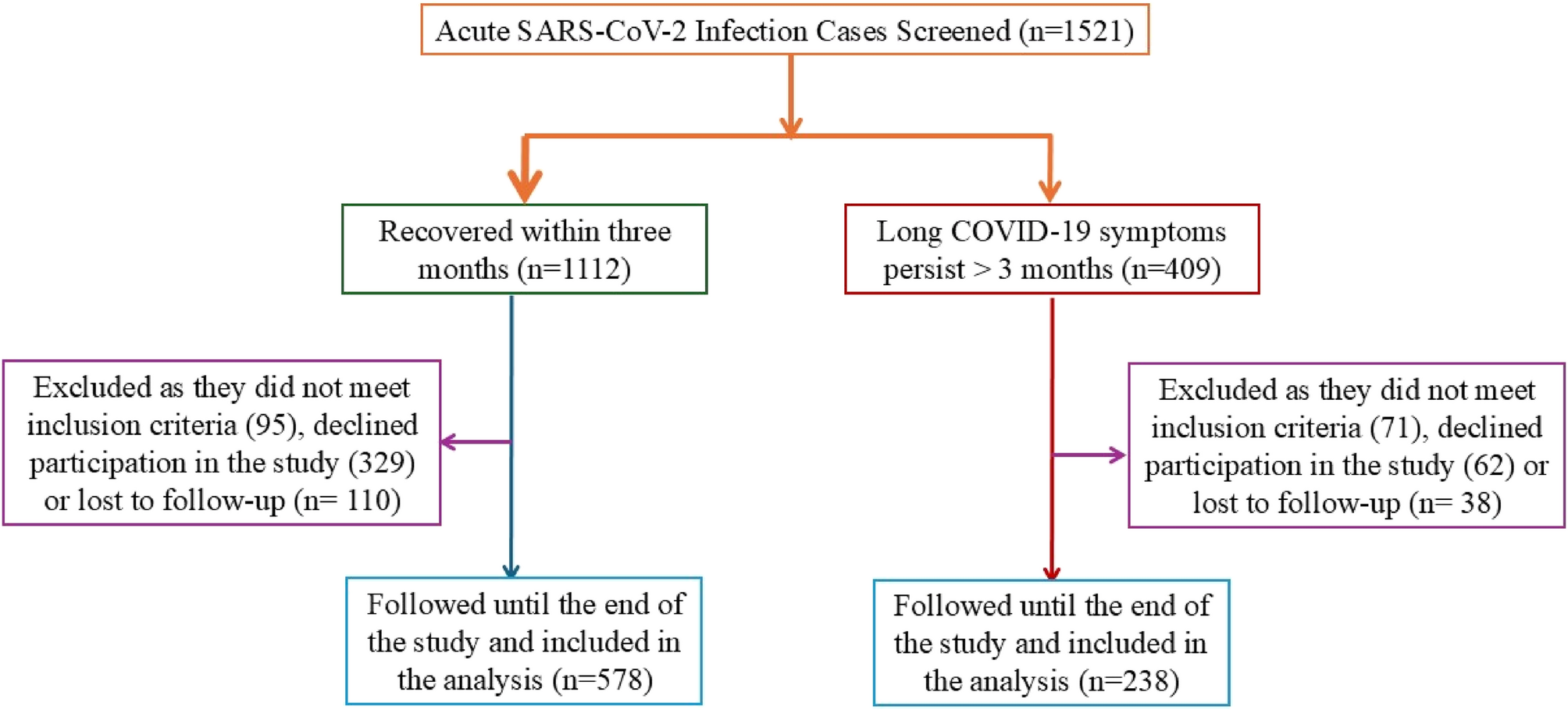
In this prospective cohort study of 816 patients followed up to four years after acute COVID-19, approximately 29% met the WHO criteria for long COVID-19. This finding is consistent with the higher prevalence estimates reported globally and highlights the long-term burden of post-acute COVID-19 symptoms. Our study offers several vital contributions: it provides one of the longest prospective follow-ups of long COVID-19 to date. It contributes new longitudinal insights by following patients for up to four years, highlighting the sustained burden of long COVID-19 not only in an underrepresented Middle Eastern and Asian population. Additionally, by evaluating the effects of reinfection and varying vaccination statuses on recovery, we provide a more nuanced understanding of long COVID-19 risk factors and recovery patterns, which may inform post-COVID care strategies in similar populations.
Our cohort had a relatively young average age (mean 41.3 years), reflecting the underlying population demographics and workforce composition of the study region, which is characterized by a predominance of younger, working-age adults. This demographic profile may partially explain differences in symptom prevalence and recovery trajectories compared to older European cohorts, where age-related comorbidities are more common.
Our cohort’s most frequently reported symptoms included fatigue, post-exertional malaise, cognitive dysfunction, and respiratory complaints. These findings mirror those reported by Sigfrid et al. and Walker et al., who similarly identified fatigue and neurocognitive symptoms as dominant and persistent features of long COVID-19 [23, 24]. In our cohort, fatigue and cognitive dysfunction persisted for over 32 weeks in some individuals, while symptoms such as cough and anosmia resolved more quickly. Our analysis adds to the existing literature by demonstrating that diabetes mellitus and female sex were independently associated with developing long-COVID-19. These associations are consistent with previously published findings by Xie et al. [25], Rathmann et al. [26], Liu et al. [27], and Ayoubkhani et al. [28], who have collectively reported that metabolic dysregulation and sex-specific immune responses may predispose individuals to prolonged post-acute symptoms. Xie et al. [25] also reported an increased incidence of new-onset diabetes following SARS-CoV-2 infection, further emphasizing the bidirectional relationship between COVID-19 and glucose metabolism.
Neurological manifestations in our cohort extended beyond cognitive complaints and included cranial nerve involvement and isolated unilateral vocal cord paralysis. Although rare, uncommon sequelae are increasingly reported and may reflect neuroinflammatory or neurovascular mechanisms in the aftermath of COVID-19 infection [29, 30]. Our findings highlight the need for tailored rehabilitation strategies for symptom-specific recovery trajectories.
In the multivariable analysis, female sex and diabetes mellitus emerged as the only independent predictors of long COVID-19. The association between female sex and increased risk is consistent with previous studies and may reflect sex-specific differences in immune function, hormonal regulation, or healthcare-seeking behavior [25, 26]. Interestingly, the effect size for female sex was modest in the univariate analysis but markedly increased after adjustment (aOR 11.11). This finding likely reflects confounding by comorbidities such as diabetes and hospitalization, which were more common among males in our cohort and may have masked the independent effect of sex in the unadjusted model. After controlling for these factors, the strong independent association of female sex with long COVID became evident, supporting a potential biological or immune-mediated mechanism rather than differences solely attributable to comorbidity profiles. The strong effect size observed for diabetes mellitus (adjusted OR 14.3) underscores the possible role of metabolic dysregulation in impairing post-viral recovery mechanisms [27, 28].
Although several variables, such as advanced age, smoking, elevated BMI, and acute illness severity, were significantly associated with long COVID-19 in the univariate analysis, they remained insignificant in the multivariate model. This attenuation of significance likely reflects collinearity or confounding by stronger predictors, notably female sex and diabetes mellitus, which emerged as independent risk factors. For instance, hospitalization and illness severity may function more as mediators of risk rather than direct predictors, with their effects partially captured by comorbidities such as diabetes. Comorbidities such as chronic renal and pulmonary diseases, which exhibited high odds ratios in the univariate analysis, lost statistical significance after adjustment, reflecting confounding by age and cardiometabolic conditions and potential mediation through acute illness severity. Exploratory interaction analyses between sex and age showed no significant interaction, confirming that female sex remained an independent risk factor across all age groups. These findings are consistent with other studies [26,27,28] and underscore the complexity of modeling long COVID-19 risk, where interdependent clinical factors can mask individual effects in multivariable analyses.
Importantly, risk factors for developing long COVID-19 did not completely overlap with those for prolonged recovery once long COVID-19 was established. Using a Cox proportional hazards model, we found that female sex, diabetes mellitus, reinfection, and hospitalization during acute illness were independently associated with delayed recovery, whereas age ≥ 60 years and chronic pulmonary disease were insignificant after adjustment. These differences likely reflect distinct mechanisms: while female sex and diabetes consistently influence both susceptibility and recovery, hospitalization may act as a marker of severe acute organ injury, prolonging recovery rather than increasing initial risk. Similarly, reinfection may exacerbate symptoms or trigger relapses in patients already affected by long COVID, but its role in initiating long COVID appears limited after adjustment for other risk factors. These observations emphasize that risk factors for developing long COVID and those sustaining prolonged symptoms overlap but are not identical, representing different stages of disease pathophysiology.
Vaccination status showed a protective trend in the time-to-recovery model. However, it did not reach statistical significance, possibly due to variability in timing, vaccine type, or waning immunity, as suggested in prior studies [14, 15]. The declining prevalence observed across enrollment periods may reflect increased vaccine coverage and/or reduced virulence of later SARS-CoV-2 variants, consistent with emerging global trends. Although variant-specific genomic data were unavailable in all our cohort patients, we stratified participants into four enrollment periods to approximate the impact of evolving epidemiological and immunological factors. Our data cannot directly attribute causality to specific variants; however, the trend parallels published findings showing a reduced risk of long COVID with vaccination and infections occurring during Omicron-dominant periods.
Our study also evaluated functional and quality-of-life outcomes using the SF-36 and EQ-5D-5 L instruments. Patients with long COVID-19 had significantly lower scores across all domains at 6 and 12 months, and only 38.7% had returned to work within one year, compared to 82.3% in the resolved group. These findings are consistent with prior studies reporting persistent fatigue and reduced quality of life in long COVID-19 survivors [10, 17]. Such substantial functional limitations warrant systematically integrating post-COVID care services into existing healthcare frameworks. Fatigue, neurocognitive impairment, and psychological distress appeared to be particularly limiting, suggesting that multidisciplinary rehabilitation, encompassing physical, psychological, and occupational support, may be essential for long-term recovery.
Our estimated long COVID-19 prevalence of 29.2% should be interpreted in the context of a hospital-affiliated cohort that included a high proportion of patients with pre-existing comorbidities and more severe acute infections, including hospitalized cases. Consequently, this prevalence may overestimate the burden observed in community-based or younger, healthier populations. Indeed, several population-based studies have reported lower prevalence rates, reflecting differences in baseline health status, healthcare-seeking behavior, and case ascertainment. Our findings, however, are particularly relevant for healthcare systems serving similar high-risk populations, such as tertiary care centers and regions with a high burden of metabolic comorbidities.
Although our findings support early identification of individuals at higher risk, such as women and those with diabetes, we acknowledge that our study is observational and cannot establish causality. While these risk factors may serve as useful markers for follow-up, interventional studies are required to determine whether tailored interventions improve long-term outcomes in these subgroups. We also explored potential interactions (e.g., between diabetes and vaccination or sex and age), but no significant modifying effects were observed. The stability of these associations across vaccination and age subgroups further supports the robustness of our findings and aligns with other long COVID-19 cohorts, where female sex and diabetes have consistently emerged as independent risk factors regardless of demographic or immunological strata [31, 32].
Several limitations should be acknowledged. First, although symptom and QoL assessments were conducted prospectively, they relied partly on self-report and may be influenced by recall or response biases. Second, we did not perform formal neuropsychological testing to objectively quantify cognitive deficits, which may have led to underestimation or misclassification of neurocognitive symptoms. Future studies should incorporate comprehensive neuropsychological evaluations to better represent long-term cognitive sequelae, as demonstrated in some studies using standardized cognitive assessment [33, 34]. Third, we did not collect biomarkers or virologic data to explore mechanistic pathways (e.g., autoimmunity and persistent viral load), although such investigations are ongoing in parallel studies. Fourth, while enrollment spanned four years, allowing long-term insight, temporal shifts in circulating variants, vaccination policy, and public health interventions may have introduced heterogeneity. Lastly, the study was conducted in a single national setting, which may limit generalizability to other healthcare systems.
In conclusion, this study provides one of the longest and most comprehensive prospective evaluations of long COVID-19 to date in the Middle East. Nearly one-third of acute COVID-19 patients in our cohort developed long-term symptoms, most commonly fatigue and cognitive dysfunction. Female sex and diabetes mellitus were independent predictors, while reinfection and hospitalization were associated with delayed recovery. The observed prevalence of 29.2% aligns with the upper range of global estimates. Importantly, this burden persists despite Saudi Arabia’s early and efficient public health response, which included nationwide screening from the onset of the pandemic and initiation of vaccination programs as early as December 2020, with substantial efforts to ensure high vaccination completion rates.
Given the young population structure and high prevalence of diabetes in the Kingdom, these findings underscore the need to integrate post-COVID care into national health systems, establish multidisciplinary long COVID clinics, and develop population-specific risk stratification tools. Our findings support early identification of at-risk individuals—particularly those with diabetes and female patients—to enable timely interventions such as structured rehabilitation programs, cognitive behavioral therapy, glycemic control optimization, mental health support, and close clinical monitoring through post-COVID care pathways. However, these observational findings do not establish causality; prospective interventional trials are needed to determine whether risk-specific management strategies can modify long COVID-19 outcomes.