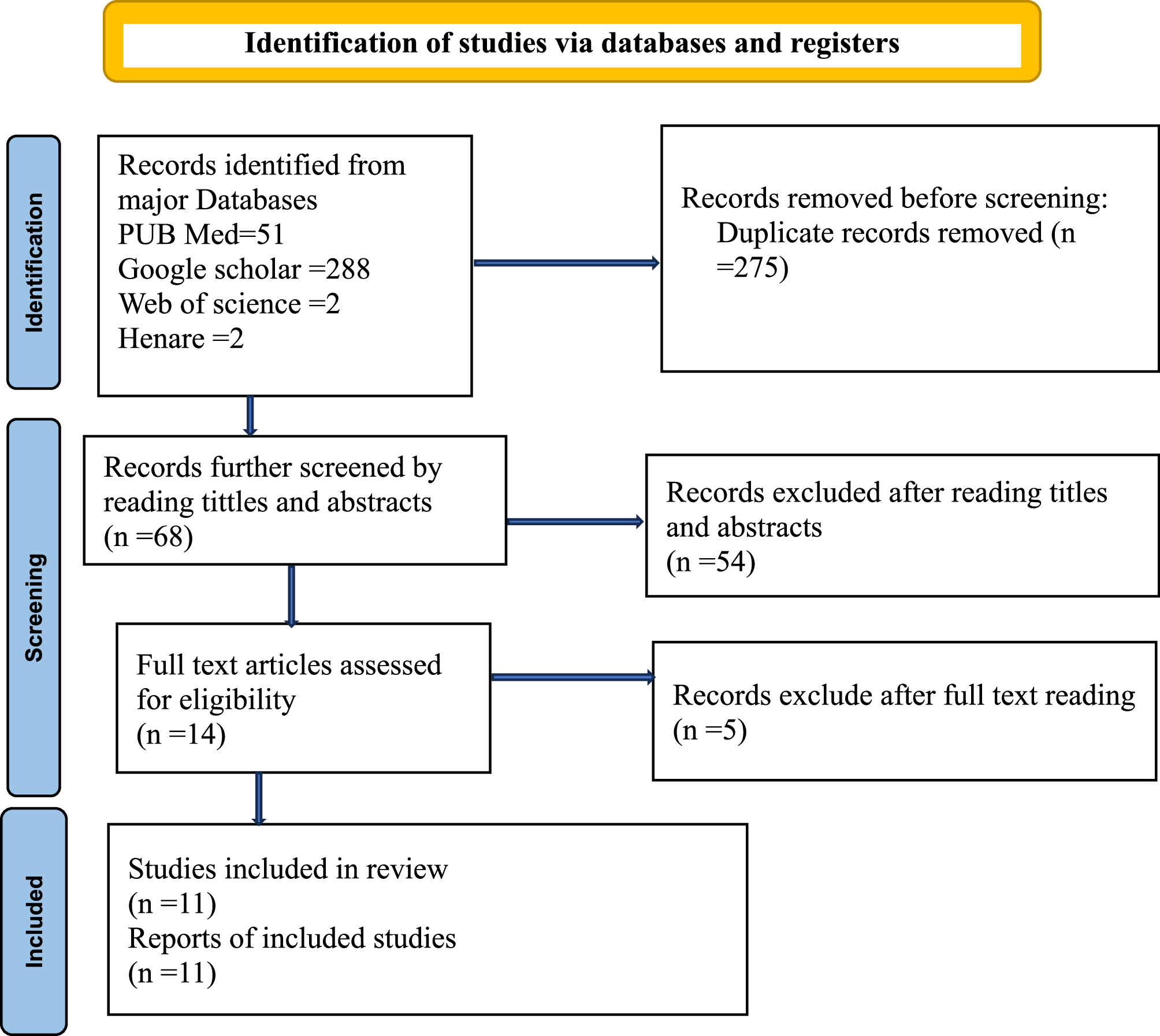
Systematic reviews and meta-analyses (SRMAs) are essential tools for addressing clinical and epidemiological questions. However, when multiple related questions within a specific topic need to be synthesized, umbrella reviews offer a practical and comprehensive approach by consolidating evidence from multiple SRMAs. This umbrella review is the first to assess cervical cancer screening uptake and its associated factors among eligible women in Africa, based on findings from 11 SRMAs. The pooled prevalence of screening utilization was found to be 19% (95% CI: 12–25%), with substantial variability across studies, ranging from 8.11 to 41%. Subgroup analyses indicated that factors such as publication year, sample size, and HIV status contributed to this heterogeneity. Notably, key determinants of screening uptake included knowledge of cervical cancer screening, perceived susceptibility to the disease, and formal education. Women with higher levels of knowledge, greater perceived risk, and formal education were more likely to utilize screening services.
The observed screening rate of 19% aligns with those reported in other low- and middle-income countries, such as Saudi Arabia [30] and Nepal [31] where similar barriers—limited awareness, cultural stigma, and restricted access to healthcare—impede utilization. These findings highlight the persistent challenges in increasing screening coverage in resource-limited settings and underscore the need for context-specific interventions to enhance awareness and accessibility. To provide a more comprehensive and balanced interpretation of our findings, we have incorporated a regional comparison, drawing on evidence from studies conducted in Europe, America, Asia, and the Middle East. This broader perspective allows us to contextualize our results within global patterns and highlights both regional similarities and disparities, thereby aligning with the regional analysis framework of our study. Compared to our findings, screening uptake is markedly higher in high-income regions: 75.2% in the United States [32], 80.15% in the Western Pacific Region, and 74.66% in the European Region [33]. These higher rates are often attributed to robust healthcare systems, organized national screening programs, and higher levels of health literacy [34]. In contrast, our result is comparable to rates reported in the South-East Asia Region (17.71%) and the Eastern Mediterranean Region (16.99%) [33], and also consistent with figures from the Middle East (18.2%) [30]. Screening coverage in African countries remains lower than global averages [33] and significantly lower than in countries such as Austria [31] Hungary [35] Russia [36] and Germany [37]. This disparity reflects structural challenges such as weak health infrastructure, socio-economic constraints, and insufficient public awareness [38, 39]. Notably, the screening rate observed in our study exceeds that of India [40] where coverage remains as low as 5%. This difference underscores the regional variability that exists even among low-resource settings, potentially reflecting more effective awareness initiatives and greater international support in certain African contexts. Such disparities emphasize the urgent need for targeted interventions in Africa aimed at improving healthcare access, strengthening educational efforts, and addressing socio-cultural barriers to enhance cervical cancer screening uptake.
This umbrella review, which synthesized evidence from 11 systematic reviews and meta-analyses, identified key factors influencing cervical cancer screening utilization in 9 of the included reviews. These factors include formal education, government employment, adequate knowledge of cervical cancer screening, history of sexually transmitted infections (STIs), perceived susceptibility and severity of the disease, perceived barriers, self-efficacy, receipt of medical advice, favorable attitudes, and perceived benefits of screening.
Women with formal education were found to have 1.85 times higher screening utilization compared to those without. Education enhances health awareness, facilitates access to and understanding of health information, and improves health literacy. It empowers informed decision-making, encourages proactive health-seeking behavior, and helps overcome cultural and social barriers. Additionally, educated women often enjoy better socioeconomic status, enabling them to afford healthcare and prioritize preventive measures [38]. This finding aligns with studies conducted in Austria [31]. Hungary [35] and India [40] But it is lower than the results from Germany [37] and Russia [41]. The higher rates in Germany and Russia may stem from more comprehensive healthcare systems, widespread screening programs, and effective public health education campaigns that boost screening uptake regardless of educational background.
Government-employed women are twice as likely to utilize cervical cancer screening compared to their counterparts. This can be attributed to better healthcare access through insurance and workplace programs, financial stability, exposure to health campaigns, supportive workplace policies, and higher education levels that enhance health literacy and proactive health-seeking behavior [42]. This finding aligns with systematic reviews and meta-analyses conducted in Nepal [43] a systematic review and meta-analysis study from Arab countries [30]. However, our finding was lower than a study done in Russia [36] and Spain [44] where higher screening rates among government-employed women are likely due to more robust healthcare access as an employment benefit, effective public health campaigns, and workplace policies promoting preventive care. Cultural factors and greater awareness may also encourage proactive health behaviors. In contrast, a study from Nepal [45] reported higher screening odds among unemployed women, possibly reflecting different healthcare priorities or support mechanisms in that context. Meanwhile, infrastructural challenges and less-developed workplace health initiatives in Africa may limit screening utilization among employed women.
Women with a history of STDs are 1.7 times more likely to utilize cervical cancer screening compared to those without such a history. This could be attributed to their increased interaction with healthcare services, heightened awareness of reproductive health risks, and the likelihood of receiving recommendations from healthcare providers during STD management to undergo cervical cancer screening [46]. This finding agreed with two independent studies done in Saudi Arabia [30, 47]. and Nepal [45].
Women with high perceived susceptibility are 1.8 times more likely to undergo cervical cancer screening than their counterparts. This heightened risk awareness, often stemming from health education, personal or family illness experiences, and healthcare provider guidance, motivates preventive action [38]. Our findings align with studies from Jordan [48] Saudi Arabia [30] Iran [49] and Spain [44] highlighting the universal role of perceived susceptibility in promoting screening. Regardless of cultural or geographic differences, recognizing vulnerability, driven by education, counseling, and illness exposure, consistently enhances screening uptake.
Women who perceive cervical cancer as a serious health threat are twice as likely to utilize screening compared to their counterparts. This heightened sense of severity increases awareness of the disease’s potential consequences, motivating women to seek regular screenings as a preventive measure [50]. Our findings align with studies from Serbia, Nepal, and Saudi Arabia. Still, they are lower than those reported in Serbia [51] Nepal [45] and Saudi Arabia, but are lower than those reported in Germany [37] Russia [36] the SRMA study and cross-sectional study in Europe [52, 53] as well as a global study [33]. These differences may stem from variations in healthcare systems, accessibility, and organized screening programs. Socioeconomic disparities, cultural beliefs, limited awareness campaigns, and financial barriers in our study setting likely contribute to lower screening rates. Methodological differences, lack of insurance coverage, and variations in education and healthcare exposure may also explain the observed disparities.
Women with low perceived barriers are 2.3 times more likely to utilize cervical cancer screening than those with high barriers. This is likely due to fewer psychological, social, or logistical challenges, improving accessibility and confidence in the screening process. In contrast, high perceived barriers, such as fear, stigma, financial constraints, and lack of awareness, often lead to delays or avoidance of screening. Consistent with behavioral health models, reducing barriers enhances preventive care engagement [54]. Our findings align with studies from Nepal [43] Saudi Arabia [30] Iran [49] Russia [36] and Spain [44] highlighting the role of improved access, affordability, and proximity in encouraging screening uptake. Effective education campaigns, positive healthcare experiences, and supportive social environments boost awareness and normalize screening practices. These consistent results across diverse settings underscore the universal need for accessible services, targeted education, and supportive policies to reduce barriers and promote cervical cancer screening.
Women with high perceived self-efficacy are twice as likely to undergo cervical cancer screening, as they feel confident in managing their health and overcoming challenges. This aligns with behavioral theories, such as Bandura’s self-efficacy theory, which links confidence in personal abilities to proactive health behaviors. High self-efficacy enables women to navigate barriers, seek resources, and prioritize preventive care [54].
Our findings are consistent with studies from Nepal [43] a systematic review and meta-analysis study from Arab countries [30] But they are lower than those reported in China [55] and France [56]. These differences may be due to variations in healthcare systems, cultural norms, awareness campaigns, and access to screening services. Higher public health education, extensive insurance coverage, and well-established screening programs in China and France likely enhance self-efficacy and screening rates. In contrast, limited access, cultural stigma, and lower health literacy in the study setting may contribute to the comparatively lower rates.
Women who receive advice on cervical cancer screening are 1.8 times more likely to utilize screening services, underscoring the critical role of healthcare providers’ counseling in promoting screening uptake. This finding aligns with studies from Japan [57] Italy [58] England [59] France [56] and two independent studies in China [55, 60]. Counseling raises awareness, addresses barriers such as fear and misconceptions, and offers tailored guidance, promoting preventive actions. Evidence from diverse cultural contexts underscores the universal significance of provider-driven advice in fostering health-seeking behaviors [61].
Women with a favorable attitude toward cervical cancer screening are 1.7 times more likely to utilize screening services than those with an unfavorable attitude. This highlights the impact of positive perceptions and beliefs on health-seeking behavior. Favorable attitudes stem from greater awareness, trust in screening benefits, and reduced fear or stigma, emphasizing the importance of targeted interventions to encourage positive views on cervical cancer prevention [62]. Our findings are consistent with studies from China [60] Italy [58] Nepal [43] Saudi Arabia [30] and Iran [49]. Strengthening awareness campaigns, dispelling misconceptions, and fostering trust in screening services can promote positive attitudes and increase screening uptake.
Women who recognize the benefits of cervical cancer screening are 1.93 times more likely to utilize screening services than those who do not. This may stem from increased awareness, reduced fears and misconceptions, and a stronger motivation for proactive health-seeking behavior. Understanding these benefits also fosters trust in healthcare systems and may inspire women to promote screening within their communities, creating a supportive environment and encouraging others to participate [63]. Our findings align with studies from Saudi Arabia [30] Iran [49] Japan [57] Germany [37] and a systematic review and meta-analysis study from Arab countries [30]. Strengthening education campaigns to highlight the benefits of screening can enhance awareness and trust, reduce barriers, and foster community advocacy, ultimately improving cervical cancer screening uptake.
In conclusion, this umbrella review highlights the low cervical cancer screening uptake among eligible women in Africa, with a pooled prevalence of just 25%. Key factors influencing screening utilization include education, employment status, knowledge of cervical cancer, history of STDs, perceived susceptibility and severity, self-efficacy, medical advice, and attitudes toward screening. Despite regional variations, common barriers, such as cultural stigma, limited healthcare access, and low awareness, contribute to this low uptake. Subgroup analyses further emphasize the need for tailored interventions, mainly focusing on education, self-efficacy, and raising awareness of the benefits of screening. To improve screening rates, it is crucial to implement targeted health education programs, enhance access to affordable services, and address cultural and psychological barriers. Policy initiatives should support community-based campaigns, healthcare provider counseling, and organized screening efforts to foster proactive health-seeking behavior and ultimately reduce cervical cancer-related mortality in low-resource African settings.
Strengths and limitations
The risk of bias was minimized through a comprehensive search across multiple databases, with four researchers independently selecting studies and a fifth resolving discrepancies. The inclusion of a relatively large number of studies enhances the robustness of the findings. Methodological quality was assessed using the AMSTAR-2 tool, and data overlap among primary studies was carefully reviewed to ensure transparency. While some overlap is inherent in umbrella reviews, it was minimal in this study, as most primary studies were unique to specific systematic reviews.
However, combining data from multiple meta-analyses may still introduce bias and potentially overestimate the strength of the findings. Moreover, due to the substantial heterogeneity across studies (I² = 100%), the generalizability of the pooled estimates is limited, and the results should be interpreted with caution. Additionally, although this umbrella review incorporated systematic reviews and meta-analyses from different regions of Africa, the majority of the included studies were conducted in Ethiopia. While these studies involved varied populations—including HIV-positive individuals, healthcare professionals, and the general population—the geographic concentration may affect the representativeness of the findings for the entire African continent. Therefore, caution is warranted when interpreting the findings in the context of all African countries.