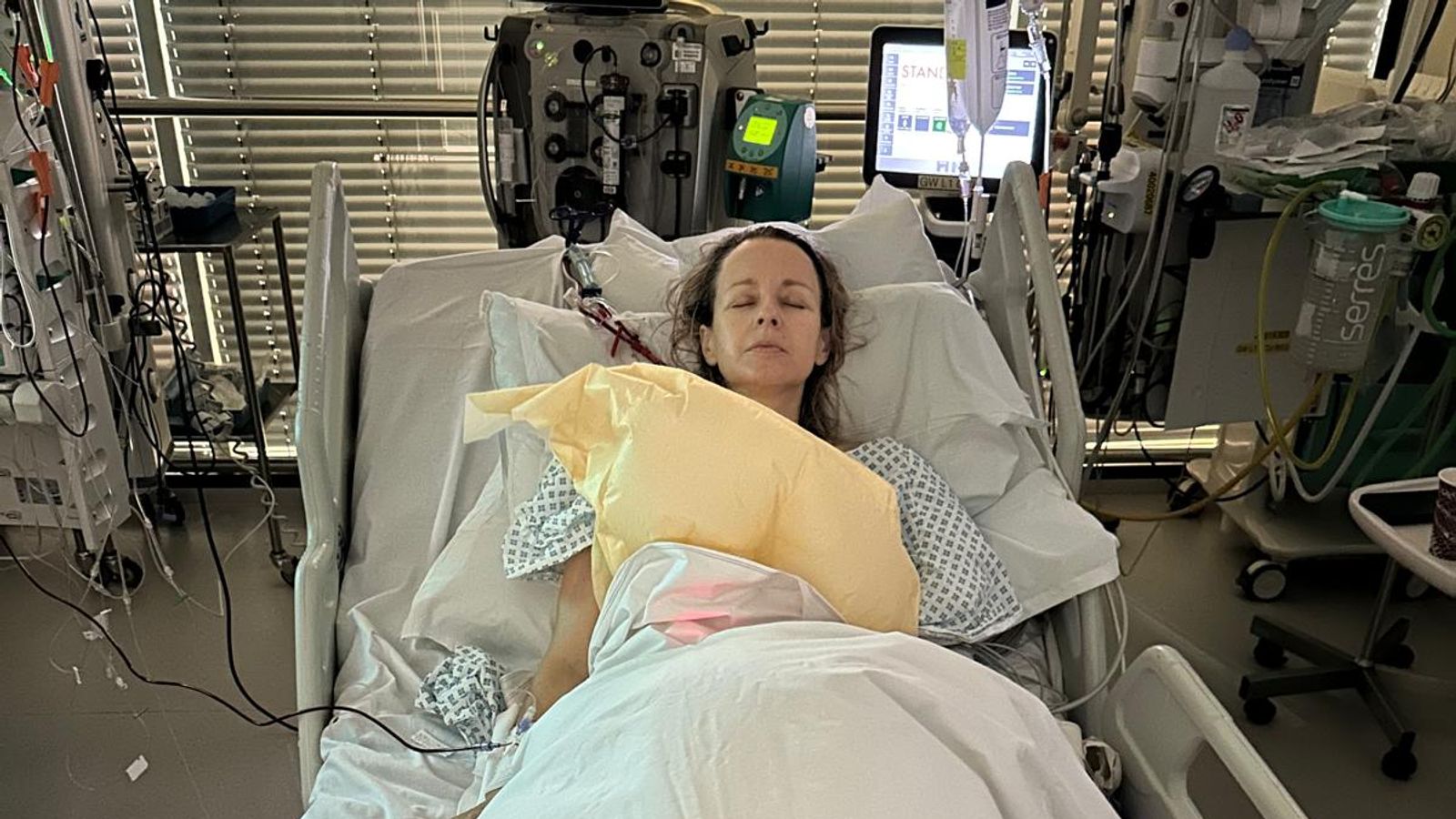
Paddling in a bay on the tiny Channel Island of Sark, I suddenly felt very sick and cold.
Less than 48 hours later, I was being emergency evacuated to the intensive care unit of a London hospital via cart, tractor, lifeboat, private jet and ambulance.
Ultimately, an incredible team of doctors, nurses, and volunteers saved my life – for a second time, though falling ill with one of the rarest diseases in the world while in one of the remotest corners of the British Isles was an unfortunate first.
I have something called atypical Haemolytic Uremic Syndrome (aHUS) that – when triggered – affects my immune system, destroying blood cells and harming other vital bodily functions.
Classed as “ultra-rare”, there is only around one new incident of aHUS per two million people every year. And an attack can be fatal, so the speed of diagnosis is key.
In my case, I already knew about the condition as I first fell ill with it eight years ago.
When it happened a second time, the heroic efforts of Sark’s only doctor, a group of volunteer rescuers and the medics at University College Hospital (UCH) meant I was raced from the middle of the English Channel to an intensive care bed in just over 11 hours – enabling rapid and effective treatment.
Now back home and expected to make a full recovery, I thought I would share my experience to help raise awareness about this little-known disease as today is aHUS Awareness Day.
‘I was feeling increasingly wretched’
My husband and I had planned to spend a few days in August on Sark – a beautiful island in between the UK and France that is a designated “dark sky” area because of an absence of light pollution.
There are no public streetlights on the territory.
More relevant to this story, cars and regular ambulances are also banned.
Instead of driving, Sark’s just over 500 residents and ferry-loads of tourists either walk, cycle or sit on the back of carts towed by horses – and on occasion tractors – to visit beaches, coves and other attractions.
I started to feel queasy on the ferry that took us to Sark.
We initially thought it was seasickness.
But the nausea lingered as we walked from the port to our hotel to dump our bags.
Thinking a swim might make me feel better, we trekked down a steep path to the beach and ventured into the sea, which is when my body decided to break.
I came out of the water, shivering uncontrollably and thought I was going to faint. After getting myself dry, we tried to return to the hotel, but I started vomiting violently on the side of the path – much to the disgust of a family that was trying to overtake us.
Once back at the hotel, I collapsed into bed, only leaving it to be sick.
We speculated that it must be food poisoning and hoped it would pass within a day.
But 24 hours later, while I had stopped vomiting, I was feeling increasingly wretched and beginning to wonder whether it could be aHUS again.
‘The onslaught is like an invisible storm’
The only other time I have been struck down by the disease was in January 2017, while working as the defence editor at The Times.
On that occasion, I took myself to my local hospital in Kent to be told that I had acute kidney failure and my bloods were “deranged”.
Fortunately, the haematologist on duty had been aware of aHUS – then a new acronym for me – and had me rushed to University College Hospital in London, which has a specialist team that can treat the condition led by Professor Marie Scully, a world-renowned expert.
I soon learnt that aHUS is caused by part of my immune system – called the complement system – becoming overactive and attacking my body rather than targeting bugs.
This “friendly fire” – likely linked to a genetic glitch that, in my case, had thankfully lain dormant for the first 40 years of my life – can be activated by infection, pregnancy or food poisoning, though sometimes the cause is unknown.
The subsequent onslaught is like an invisible storm that destroys a patient from the inside, shattering red blood cells, damaging small blood vessels and causing tiny clots.
The clots clog up kidneys and trigger acute renal failure.
If left untreated, other organs can also collapse, while the risk of a stroke or heart attack rises.
Without intervention, the prognosis is dire.
Between 10 to 15% of patients die during the initial illness, while up to 70% of patients develop end-stage renal failure, requiring a lifetime of dialysis.
Since 2013, however, patients in the UK have had access to a drug called eculizumab, which effectively turns off the malfunctioning part of the immune system. It is expensive – at many thousands of pounds a shot – but it saves lives, including mine.
‘My protein levels were off the scale’
Lying in bed in Sark more than eight years on from the first episode, I did not want to believe my body had turned on itself again.
But after a little over 36 hours, with no improvement, my husband decided to get help.
His action likely saved me from even graver kidney damage or worse.
He set out to find Sark’s only GP, Dr Bruce Jenkins.
Blood tests are the best way to diagnose aHUS, but they were not an option on the island.
Instead, Dr Jenkins did a urine test, which is a good alternative.
Any trace of blood or protein in the urine is a sign that a person’s kidneys are in trouble.
My protein levels were off the scale of the test.
Upon seeing the result, Dr Jenkins instructed my husband to go back to our hotel and pack our bags – I was still floundering in bed – while he coordinated an emergency evacuation.
On Sark, given the lack of vehicles, this meant mobilising an ambulance cart towed by a tractor, which is operated by a team of Community First Responders – all volunteers.
The GP also contacted the main hospital on Guernsey, a larger Channel Island, which provides a marine ambulance service to rescue anyone with a medical emergency on Sark.
While all this was happening, I called an emergency number for the aHUS medics at University College Hospital to warn them I was likely suffering a relapse.
By chance, Professor Scully was on duty that day – a Friday – and over the weekend. She and her team sprang into action, contacting Sark and Guernsey to help.
Speed was key as my condition was worsening.
‘I asked a doctor if I was going to die’
Within minutes of the alert going out from Dr Jenkins, a tractor, pulling a white ambulance cart, arrived at our hotel, and the first responders guided me and my husband onboard.
They took us to the port to wait for the “Flying Christine”, an ambulance boat carrying two paramedics and operated by St John’s Ambulance and Rescue Service.
That team transported us via sea to Guernsey hospital before we were transferred to a specialist medical plane to be flown to Luton airport.
The last leg was a more conventional ambulance drive to UCH, where critical care doctors, as well as Professor Scully and her colleagues, were poised to start the treatment.
Read more from Sky News:
New dinosaur discovered
Tributes to legendary umpire
NASA accelerates moon mission plans
This quick response by the NHS and a network of volunteers meant I was taken from my sickbed in Sark to life-saving treatment in London in barely 11 hours.
By this point, the aHUS attack had caused my haemoglobin and platelet levels to drop, and my kidneys were failing.
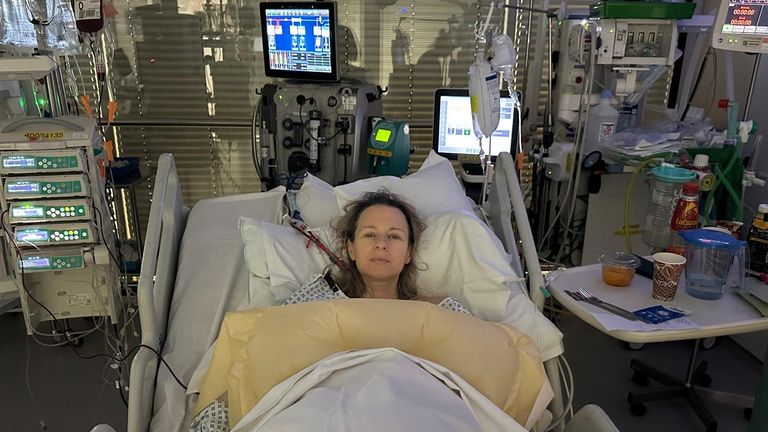
The main treatment was the eculizumab drug – administered intravenously – but I also needed blood transfusions and to be put on a machine that acts as a form of dialysis.
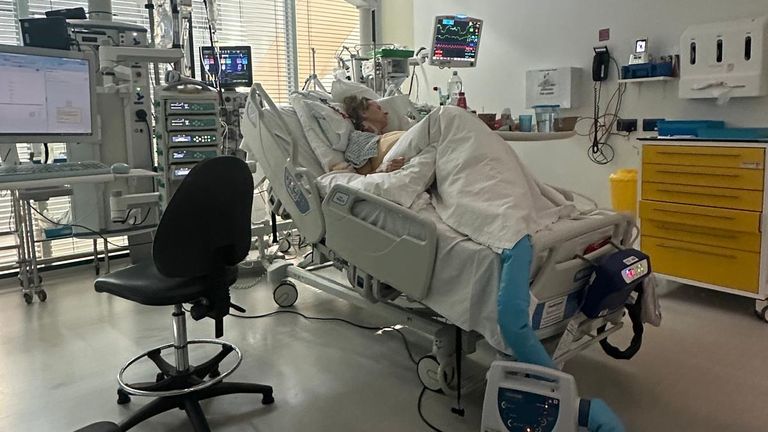
The relief of being in the best possible place for my condition was immense, but the next few days were still frightening as my body took time to respond.
At one point, I asked a doctor if I was going to die – she assured me I was not.
On another occasion, pumped full of medication, hooked up to various machines and drifting in and out of sleep, I dreamt I was under missile fire – an occupational hazard of being a journalist who covers war – and tried to leap out of bed to an imaginary shelter, prompting the nurse who was looking after me to spring into action and make sure I stayed put.
Gradually, though, the treatment started to work.
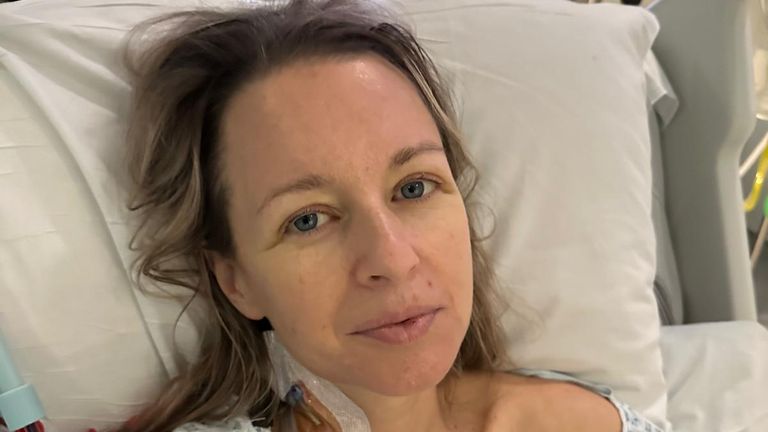
After nearly a fortnight in hospital, including one week in intensive care, I was well enough to be discharged.
Today, I am on the mend and incredibly grateful to everyone who helped to save me from myself.
Deborah Haynes and Professor Marie Scully will be on Sky News from 8.30am to speak about aHUS Awareness Day.